![]()
Patient 1:
A middle-aged woman presents with progressive dyspnea. You start with her hands. What do you notice? Does it generate any hypotheses in your mind?
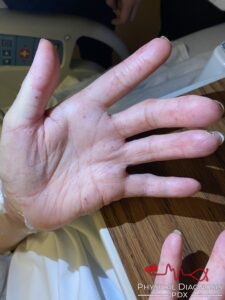
Could these small erythematous lesions be telangiectasias? Let’s see if they blanch and refill by pressing on one of them.
Indeed, they do, confirming your suspicion. What condition comes to mind? Perhaps you are thinking about hereditary hemorrhagic telangiectasia (HHT). Can it cause dyspnea? Yes, via pulmonary AVMs. What other condition can present with telangiectasias that may involve the lungs?
Your new hypothesis leads you to examine the hands further, discovering that the patient has a hard time completely straightening her fingers. You ask her to make the universal sign of prayer.
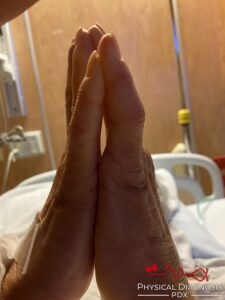
You search her skin for other signs of the condition that is now at the forefront of your mind. What is this hard, white nodule on her elbow? Does it further advance your hypothesis?
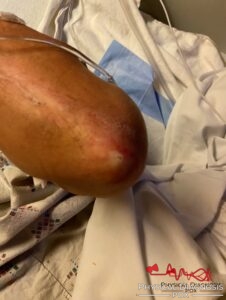
So what about the dyspnea? How does the condition you have in mind affect the lungs? You look for evidence of pulmonary hypertension on exam. You start with the jugular venous pulse. What finding is present?
Then you auscult the heart. What finding is present? What is your ultimate diagnosis?
This patient has scleroderma with systemic involvement (SSc). Typical cutaneous manifestations include telangiectasias, sclerodactyly (+ Prayer sign), and calcinosis cutis (nodule on her elbow). SSc can cause pulmonary hypertension, leading to Kussmaul’s sign and loud P2.
A standardized test would provide all of these clues on a silver platter. Any machine can synthesize them and make the diagnosis. The clinician must not only synthesize, but gather these clues at the bedside. Your search must be hypothesis-driven or you might miss them.
Anticipation is key in medicine. The eyes can’t see what the mind doesn’t know. The ears can’t hear what the mind doesn’t know.
